AI Claims Processing Software for US Carriers
From first notice of loss to a substantiated, fully documented decision in under 2 minutes. Built for the audit trail your state DOI examiner will request, the explainability your General Counsel demands, and the 10x to 50x volume spike your next CAT event will force on your claims operation.
.jpg)
What US Claims Leaders Actually Face in 2026
In our 20 years building insurance software for P&C carriers across Europe and North America, we have not seen a worse mismatch between what the market demands from claims operations and what most carriers can deliver. AI claims processing software is no longer a 2028 conversation. It is the difference between a J.D. Power top-quartile carrier and one watching renewals walk out the door.
Cycle time is now the #1 retention driver, not payout amount
J.D. Power’s 2025 U.S. Auto Claims Satisfaction Study identified claims cycle time as the strongest predictor of policy renewal in personal auto. Top-quartile carriers are settling clean auto claims in roughly 6 hours. The industry mean still sits at 3 to 7 days. Each day of delay drives NPS measurably down and renewals measurably out.
The NAIC AI Model Bulletin is no longer optional
Sedgwick’s 2026 property claims report found that between 58% and 82% of US insurers now use AI tools, yet only 12% report mature AI capabilities and only 7% have achieved scaled AI success. The gap between adoption and maturity is now a regulatory exposure. 24+ US jurisdictions have adopted the NAIC AI Model Bulletin, which requires every carrier to maintain a documented AI Systems (AIS) Program that the state Department of Insurance can request during any market conduct action.
Fragmented pilots will not bend your combined ratio
The dominant failure pattern I see in US claims operations is fragmentation: one vendor for OCR, another for fraud scoring, a third for image analysis, none of them sharing a decision audit trail. Value gets trapped in individual claim steps. Combined ratio does not move. That gap is what Claims AI was built to close.
How AI Claims Processing Software Works, End to End
When a claim arrives, Claims AI moves it through nine decision layers in roughly 90 seconds on clean submissions. Your adjuster sees only the result and the recommendation.
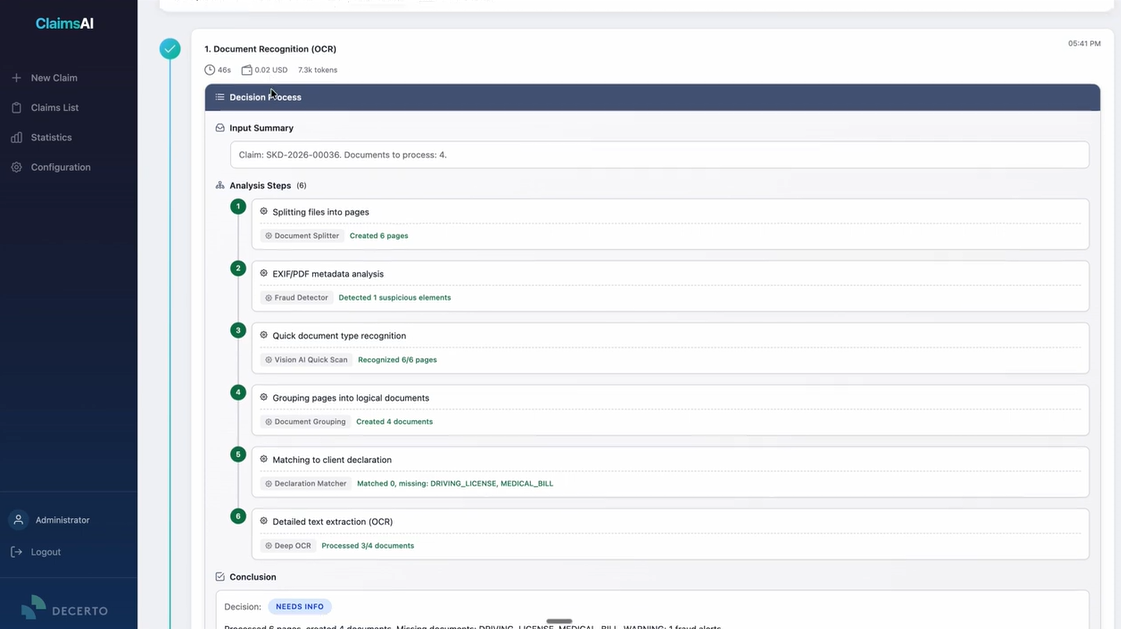
Intelligent document intake (OCR)
Claims AI ingests PDFs, mobile photos, scanned paper, and handwritten notes with over 99% extraction accuracy. The vision model describes damage in policyholder photos in natural language.
Contextual analysis (NLP)
The engine does not keyword-match. It extracts policy number, date of loss, loss type, and claimant identity, then auto-classifies the submission into one of 40+ claim categories tuned for US P&C lines.
Coverage verification against your PAS
Claims AI connects in real time to your Policy Administration System. If coverage lapsed, premiums are past due, or the loss falls outside the effective window, the claim stops here. The adjuster never sees it.
Endorsement and special-conditions retrieval
The system locates scanned endorsements and riders, including the ones that exist only on paper and were never indexed in the core. Nothing slips by.
Completeness
If the claimant has not submitted required documentation for that loss type, Claims AI auto-generates a request letter and sends it through your preferred channel (email, SMS, mailed paper).
Fraud signals at FNOL, not seven days later
Advanced metadata and EXIF analysis detects Photoshop manipulation, checks photo geolocation, and catches duplicate documents from serial claimants.
Policy wording validation
The AI agent searches your specific policy terms and conditions and pinpoints the exact clauses that support approval or denial. Every decision is grounded in your contract language, not in the model’s training data.
Claim valuation
Product-specific algorithms for personal auto, homeowners, workers’ comp, and commercial lines calculate the claim amount against impairment schedules, medical fee schedules, and invoice verification. Output is a defensible damages calculation, traceable line by line.
Adjuster-in-the-loop decision
Claims AI prepares the recommendation and drafts the correspondence letter to the claimant. The adjuster approves, edits, or overrides. A human always makes the final call before payment goes out.
This is not “AI deciding claims on its own” in the sense that worries your General Counsel. It is high-velocity decision support that lets your adjusters spend their day on the 20% of claims that actually need human judgment.
Why Decerto Claims AI?
Four properties separate Claims AI from the generic AI claims pitch deck. Each one is a structural design choice, not a feature toggle.
Compliance-first by design, not retrofitted
In the insurance world,regulatory compliance isn’t optional — it’s the baseline. Our architecture was designed to meet the most rigorous standards.
Global & State-Level Compliance: Full support for GDPR in the EU as well as CCPA, NYDFS Cybersecurity Regulation (23NYCRR 500), and other state-level privacy and insurance regulations in the U.S.
Data Sovereignty: Data stays where it belongs. We process European data in the EU and U.S. data domestically.
Full Auditability: Immutable, time-stamped logs allow you to reconstruct every step of the process — ready for DOI examinations and regulatory audits.
Human-in-the-Loop: AI supports, but a human makes the final call. Full control over the level of automation.


Multi-provider AI, no vendor lock-in
Claims AI does not bet your operation on one foundation model. We select the best model for each task: a different model for vision, NLP, fraud anomaly detection, and policy-clause retrieval.
Flexible Configuration: Switching providers is a simple config change, not a months-long code migration.
Built-In Failover: If one model goes down, the system automatically switches to an alternative, ensuring business continuity.
Insurance-native engineering team
The Claims AI team has spent 20 years implementing core insurance systems for European and North American carriers.
Domain Knowledge Baked In: We understand the nuances of policies, endorsements, and claims adjudication workflows better than any generic AI solution.
Agent Portal Experience: We leverage know-how gained from the largest core system implementations in the market.
Out-of-the-Box Integrations: The system connects instantly with your PAS (Policy Administration System) and financial/accounting platforms.


Transparent per-claim ROI: See the Savings, Not Just the Costs
You see the exact cost of processing each claim, broken down by OCR, contextual analysis, fraud scoring, and policy validation.
Full Cost Analytics: See the exact cost of handling each claim, broken down by OCR, analysis, and fraud detection.
Business Dashboards: Track time savings and system performance on a weekly and monthly basis.
Precision Scoring: Every submission receives a clear fraud-risk score, letting your adjusters focus where it matters most.
Stop Processing. Start Deciding.
Imagine a complex Personal Accident claim involving a rock-climbing injury, multiple medical invoices, and specialized policy endorsements. While a manual review would take hours, Claims AI completes the heavy lifting in just 90 seconds.
Our engine instantly executes high-precision OCR and image analysis, verifies coverage against the PAS, and deep-scans original policy documents to identify specific exclusions—like extreme sports clauses. Simultaneously, it runs a sophisticated fraud check, flagging edited EXIF metadata that the human eye might miss. The result? A fully valued $30,500 claim with a generated denial recommendation based on precise policy wording.
By the time the adjuster steps in, the entire case is ready for a final click. What used to be a half-day task is now a 5-minute closing, processed at a radical cost of just $0.05 per claim.
.png)
How a Free Claims AI POC Works (14 Days, NDA-Protected)
You are 4 steps from a working Claims AI sandbox tuned to your use case.
Used by the World's Leading Companies






FAQ
We've gathered answers to the questions we get asked most often.

AI claims processing software ingests the FNOL submission (documents, photos, structured fields), extracts the relevant data via OCR and computer vision, verifies coverage against your PAS, runs fraud signals at intake, validates against policy wording, calculates damages against schedules, and presents a substantiated recommendation to the adjuster. On clean submissions, Claims AI completes this end to end in roughly 90 seconds.

Claims AI runs on cloud-native infrastructure that auto-scales for 10x to 50x normal volume during CAT events. The practical constraint at most carriers is the integration layer, not the AI engine. We recommend running parallel-load tests in November (before the next hurricane and severe-convective-storm cycle), and avoiding go-live windows between April and October when CAT exposure peaks.

For a US P&C carrier writing $300M to $1B in direct written premium, mature Claims AI deployments produce a 25% to 40% reduction in LAE as a percentage of earned premium within 18 months, plus measurable improvement in J.D. Power claims satisfaction index. Per-claim processing cost on clean submissions drops to the $0.05 to $0.40 range depending on line complexity.

Always. Claims AI is built with human-in-the-loop as a structural property of the architecture, not as a feature toggle. The system prepares a recommendation and drafts the correspondence letter; the adjuster approves, edits, or rejects before any payment is authorized. There is no AI-only payment path outside the pre-configured STP rules you encode in Higson and govern under your AIS Program.

Yes, if it was designed for compliance from day one. Claims AI was built against the NAIC AI Model Bulletin adopted by 24+ US jurisdictions as of late 2025. Every decision generates an immutable, time-stamped audit log mapped to the AIS Program documentation requirements. Retrofitted explainability on a black-box model is expensive and produces weaker DOI documentation than systems built with audit trails as a first-class design property.

End-to-end implementation for one line of business runs 4 to 6 months with Decerto’s pre-built US P&C models. Full multi-line deployment with deep integration to your PAS, document management system, and fraud platform typically runs 11 to 14 months. Vendors quoting 18-plus months are usually starting model training from scratch, which is rarely necessary in US P&C.

A Claims Management System is the workspace where your adjusters work. Claims AI is the decision engine that surfaces the right information, runs the validation, and prepares the recommendation. They are complementary, not competing. Decerto offers both as integrated products, but Claims AI runs against any major US CMS in production today.

Claims AI ships with pre-built integrations for the major US PAS architectures, financial and accounting platforms, document management systems, and external fraud data sources including NICB and ISO ClaimSearch. For heavily customized legacy cores, we run a 2-week integration scoping session as part of the free POC, with a defined integration cost on the table before any contract is signed.
Still have questions?
If you didn’t find the answer to your question on our website, please contact us. We’ll get back to you within 24 hours.

30 Minutes with Decerto Specialist
Walk through your specific carrier stack and tell us where it hurts most. We'll tell you within the call which Decerto products solve it, what the realistic timeline is, and whether you should keep what you have. NDA signed before the call if needed.